Field Updates
Visiting Uganda by Nicole Alexander, Senior Manager, Communications
In June, I was so fortunate to see some of our projects in Uganda in person! This was my first time in Africa! Over the three-day trip, I saw our COVID-integration projects, two community clinics, and a maternity ward. Read about Day 1, Day 2, and Day 3!
Day 1: June 5th, 2023
Staff Visit
On my first day, I visited Terago, Uganda’s newest district (similar to counties here in the US), founded in 2020. The area borders South Sudan and the Democratic Republic of the Congo, and people from those neighboring countries have sought refuge for so long in Uganda that the native and refugee populations are almost one. The government doesn’t place time limits on their stay as everyone recognizes the instability of the surrounding countries and wants to do what it can to help. Even students and healthcare seekers regularly cross the borders for education and care. According to Dr. Tonny, Amref Project Manager for all fistula work in Uganda, “Since we are one people, we recognize the hostility around us and want to give what we have to offer.”
Terago has just over 500,000 people, with 29 health facilities that offer a range of services. However, there are only four doctors to serve the entire population. Because of this gap, Mr. Olema, the Acting District Health Officer who conducts disease surveillance for the district, shares how Amref Uganda’s Village Health Teams (VHTs) are essential to connecting people to care and gathering health information for the office. “Through Amref, we are so grateful for this kind of support. Our coverage was about 97%, but it’s now beyond 100% of our goal with Amref’s help. Amref helps communities get missed opportunities like other essential vaccines and WASH access.”
Immanuel, the Project Manager for the Amref Uganda: Arua Office, says that VHT members are trained to respond to and manage outbreaks, share informational materials, and walk with testing kits and tents to create triage areas to help boost efforts. There are challenges, especially as life-changing outbreaks seem to be a little more frequent now (he told us there was a measles outbreak not too long ago), so there are hopes to have an isolation center near the border and an expanded laboratory to truly be ready to handle whatever outbreak is next.
To arrive in Ofua, I had to take a small plane. Here, you can see how the area shifts from urban to rural. Photo Credit: Nicole Alexander.
Health Center Visit
After this, I traveled to Ofua to see a health center with one clinical officer, one nurse, one midwife, one lab assistant, five volunteers, three translators (the area is home to multiple languages), one guard, and one janitor. This single facility serves nearly 6,000 people, including an estimated 2,000 people who have to travel to this center because it’s the closest one.
This health center offers many services, including family planning, pre-and post-natal care, immunizations, laboratory services, and rapid testing for malaria, typhoid, HIV, and more. They can do minor surgical procedures, incision and drainage (commonly abbreviated as I&D) and treat common conditions.
A big thing done is weekly outreach, where staff go to central areas in the neighborhood to provide standard care and testing and make referrals for anyone with a more complicated case. They can even arrange transportation to the nearby hospital for severe cases. The services are available to anyone who shows up at no cost to the community. The team also does quarterly dialogues in the community to get their feedback on the services provided and what they would like from the health center or the community popup events.
For the first half of 2023, the staff’s community efforts contributed to reducing diarrhea through their WASH awareness campaigns and connected with area schools to immunize students and community members. Currently, they are working to reduce home deliveries. But, the facility doesn’t have a delivery room, and the nearest one is far away, so many women give birth at home, putting them at the highest risk of infection and even death.
I learned that a new challenge is appropriately dealing with mental health cases. Because the staff is so limited and not everyone is trained in mental healthcare, they cannot address all the cases they come across, especially if the person has special needs. This, along with infrastructure improvements like solar power, fencing, waste management, and transportation, are things they hope to get to make life safer and better for their community.
The facility is open Monday, Wednesday, Thursday, and Friday from 8 am to 5 pm and can have anywhere from 80 – 100 visitors a day. When we went, Dr. Fred, the Clinical Officer, had already seen 70 people by 3 pm!

A view of the health center! Though we arrived early in the morning, there was already a line of people waiting for services. Photo Credit: Ambrose Watanda.
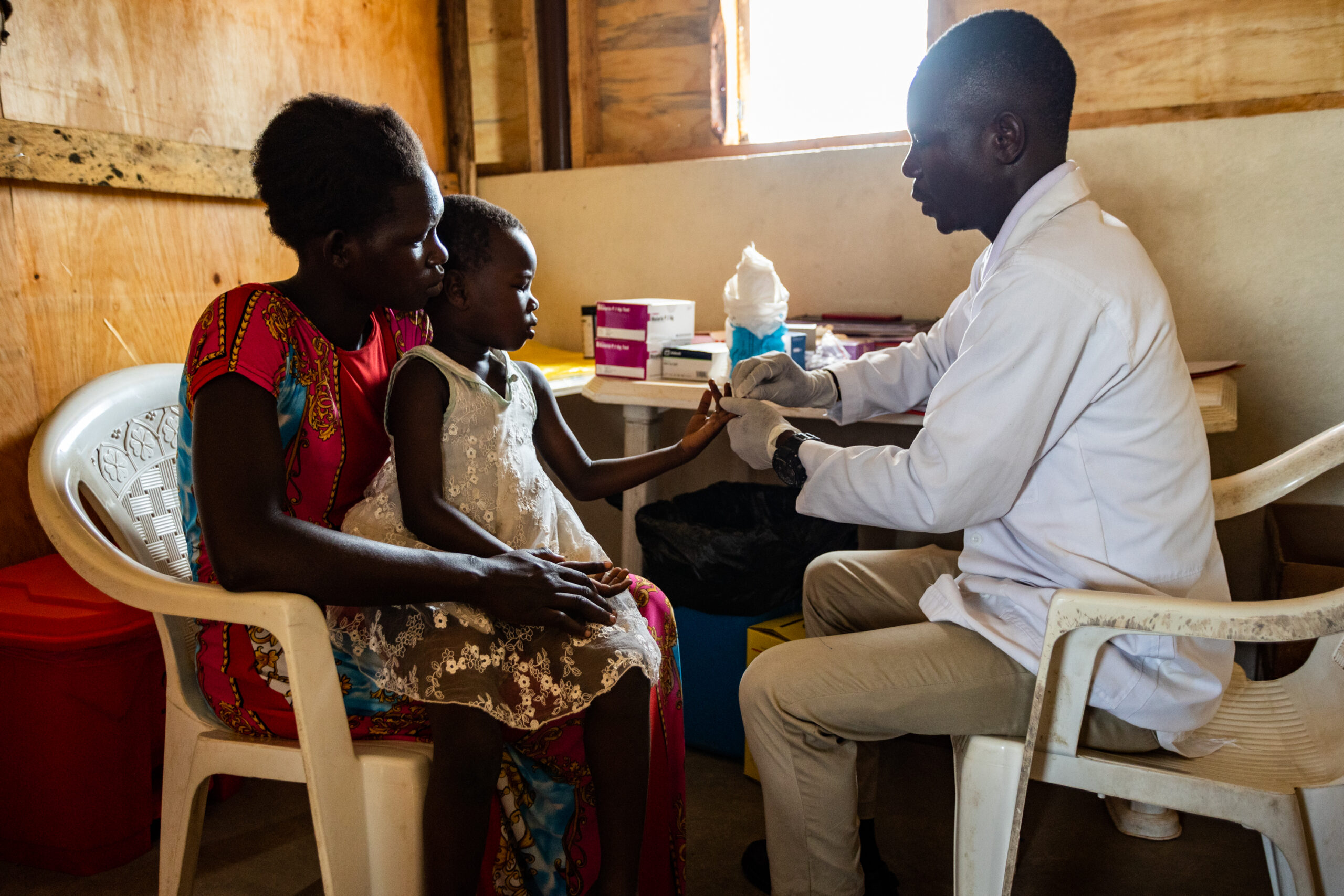
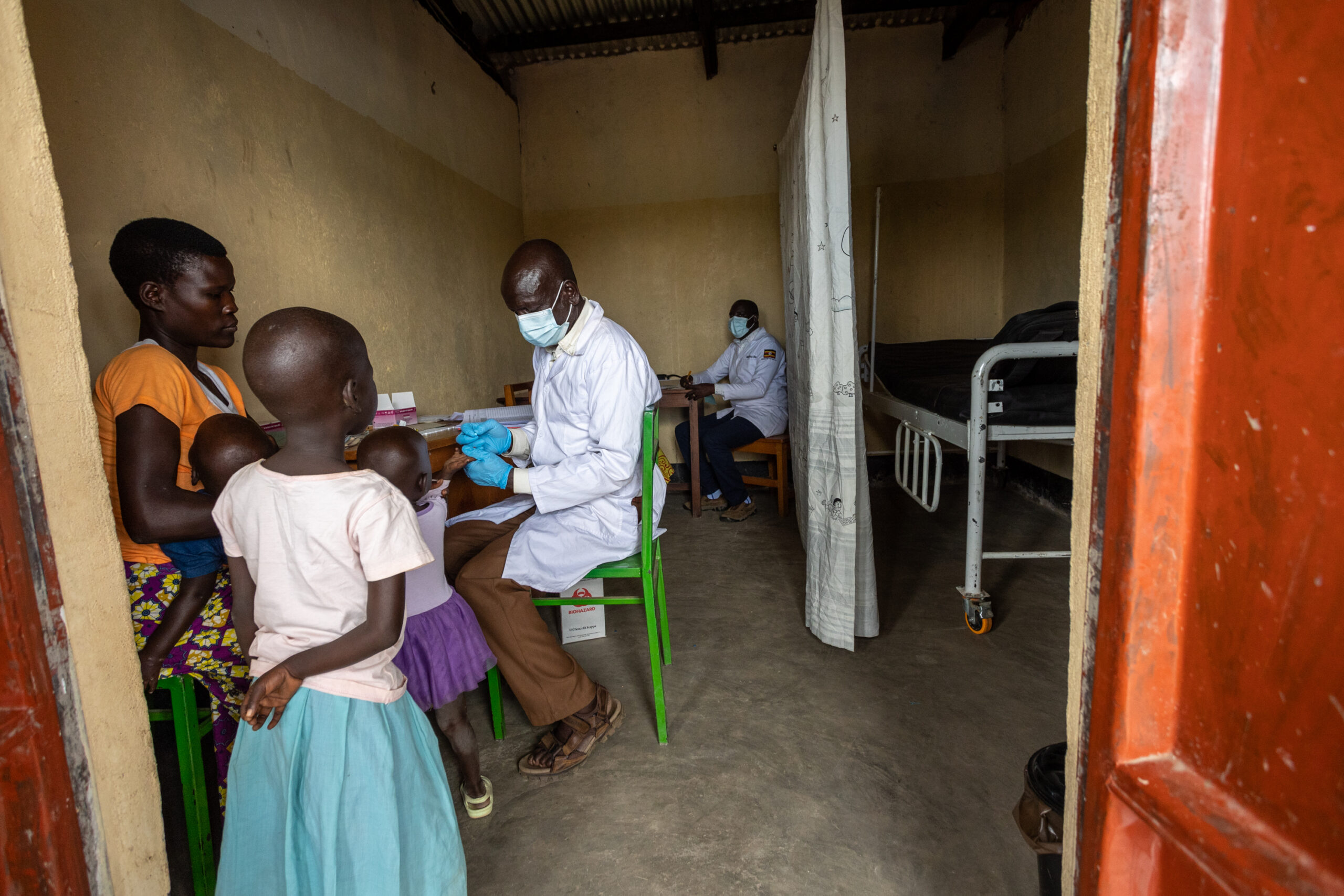
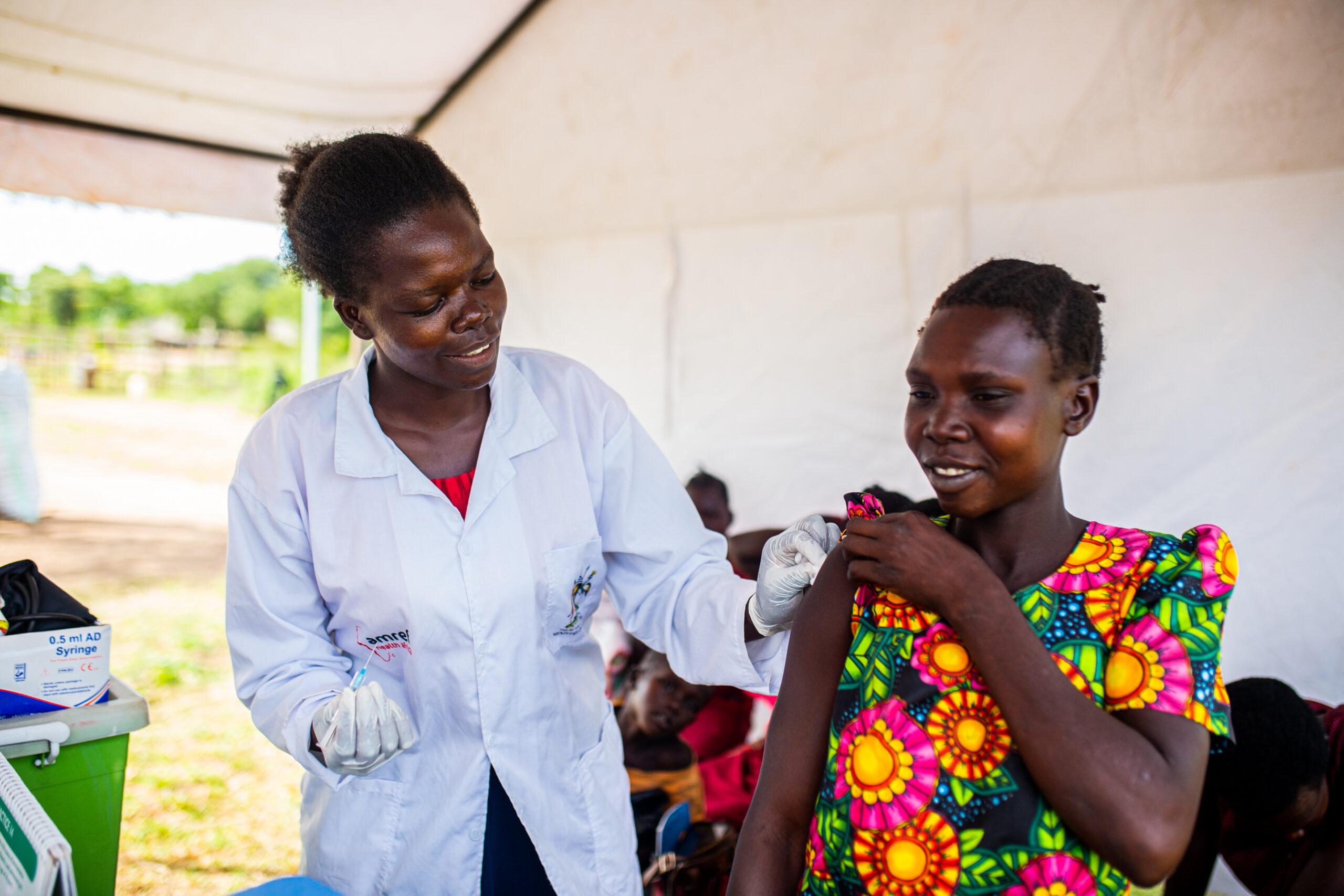
A health worker testing a young child for malaria, a mother getting all her children tested, a midwife giving a pregnant mother preventative vaccines, and a sectioned-off room for patients requiring more intense treatments. Photo Credit: Ambrose Watanda.